The Geography of Access to Health Services
According to a 1993 Institute of Medicine report, access to health services means “the timely use of personal health services to achieve the best health outcomes.” Geographic access is listed as one of three distinct components of access (along with insurance coverage and finding a trusted provider). Without adequate access to healthcare and health services, people run the risk of having their health needs unmet, sometimes delaying care in a way that lands them in a hospital when preventive care options or primary care services could have helped. Such hospitalizations often lead to enormous financial burdens that might impoverish individuals and their families or weaken the healthcare organizations that provide unpaid services. This blog post will review the geography of access to health services through its evolution of the last few decades to show how far we’ve come and to offer a glimpse into where we’re headed with the complex questions of access.
The patient perspective on access
In the early days of calculating access (not too long ago), health researchers would use their geographic information system (GIS) to calculate the Euclidean (straight line) distance from a patient’s ZIP code centroid to a healthcare facility. Even if full patient addresses were available, it could be time-consuming to perform these calculations for an entire hospital database. Although aggregating to the ZIP code level severely diminishes the value of the data, the method offered a more feasible option for those wanting to compare accessibility for various communities.
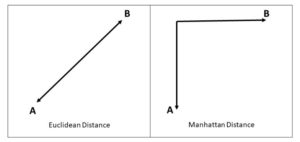 Savvy spatial thinkers recognized that the Euclidean distance calculation offered no insight into the actual distance one might travel along a road network to get to a destination, and they chose instead to employ the Manhattan distance calculation as a simulation. The method offered N–S or E–W movements in a stair-step pattern. While the resultant distance was likely more appropriate in most cases, there was no question that it was a substandard approach to calculating distance along a road network. Until recently, understanding access to care from the patient perspective has been a daunting technological challenge.
Savvy spatial thinkers recognized that the Euclidean distance calculation offered no insight into the actual distance one might travel along a road network to get to a destination, and they chose instead to employ the Manhattan distance calculation as a simulation. The method offered N–S or E–W movements in a stair-step pattern. While the resultant distance was likely more appropriate in most cases, there was no question that it was a substandard approach to calculating distance along a road network. Until recently, understanding access to care from the patient perspective has been a daunting technological challenge.
The healthcare facility perspective on access
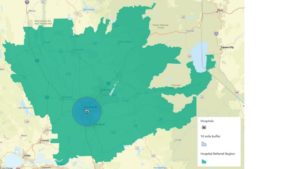 Healthcare administrators have also been interested in the issue of access. The concept has broad implications for planning services, managing populations, and preventing hospital readmissions. Initial GIS methods for access calculations from this perspective included the use of buffers or pre-defined service regions. It’s a very simple prospect to drop a point representing a hospital and create a 10-mile circular buffer to represent an area of general accessibility to the facility. From the hospital perspective, this method is roughly equivalent to the Euclidean distance calculation.
Healthcare administrators have also been interested in the issue of access. The concept has broad implications for planning services, managing populations, and preventing hospital readmissions. Initial GIS methods for access calculations from this perspective included the use of buffers or pre-defined service regions. It’s a very simple prospect to drop a point representing a hospital and create a 10-mile circular buffer to represent an area of general accessibility to the facility. From the hospital perspective, this method is roughly equivalent to the Euclidean distance calculation.
Many healthcare organizations took advantage of the work of the Dartmouth Atlas Project on accessibility. The work was groundbreaking at the time and is still used today to understand hospital service areas (HSAs) and hospital referral regions (HRRs). The former were meant to represent the area for any hospital where the greatest proportion of its Medicare residents were hospitalized. The latter were meant to represent where the greatest proportion of major cardiovascular procedures were performed. Dartmouth Atlas Project published all the various boundary layers, making it easy for organizations and researchers to download and use them for their work. For many, the expediency, as well as a de facto industry standard, was reason enough to ignore the downsides—all data were calculated for Medicare patients only, and the resultant polygons were built to increase contiguity and avoid overlap—both unrealistic accommodations of convenience.
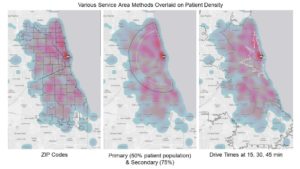 In 2000, Radke and Mu inspired the development of a method offering improved realism for accessibility called the two-step floating catchment area. The technique, derived from gravity models, attempts to capture several spatial variables and their interactions. The model requires the assessment of physician availability (supply) at locations (i.e., hospitals) as a ratio to their surrounding population (within a travel time threshold) and then sums those ratios around each residential (demand) location. Since its development, several enhancements have been made to the method that improve accuracy across different environments (like rural and urban). In 2011, a three-step floating catchment area technique was published that helped to minimize the overdemand estimation caused by the two-step method. The advance further refined the results, offering potential for better resource planning and identification of health professional shortage areas due to limited access.
In 2000, Radke and Mu inspired the development of a method offering improved realism for accessibility called the two-step floating catchment area. The technique, derived from gravity models, attempts to capture several spatial variables and their interactions. The model requires the assessment of physician availability (supply) at locations (i.e., hospitals) as a ratio to their surrounding population (within a travel time threshold) and then sums those ratios around each residential (demand) location. Since its development, several enhancements have been made to the method that improve accuracy across different environments (like rural and urban). In 2011, a three-step floating catchment area technique was published that helped to minimize the overdemand estimation caused by the two-step method. The advance further refined the results, offering potential for better resource planning and identification of health professional shortage areas due to limited access.
Nowadays, network analysis is an easier task to perform, so hospitals and other health organizations can easily create drive-time and/or drive-distance buffers. Finally, the technology aligns with the literature on health service access, which notes that both parameters (time and distance) are predictors of service utilization.
Combining patient and provider perspectives to improve access
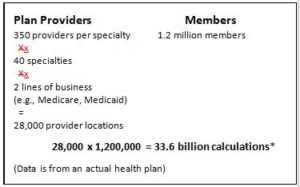 But what about going back to the patient perspective on the question of access to healthcare? There are now regulations in place that attempt to improve access to care by first understanding it from the patient’s perspective. I’m talking about network adequacy requirements, which refer to a health plan’s (including provider/plans) ability to deliver the benefits promised by providing reasonable access to a sufficient number of in-network primary care and specialty physicians, as well as all healthcare services included under the terms of the contract. Given the vast differences in topologies and road networks from one place to another, it makes sense that the regulation is based on driving times and driving distances together to formulate the most accurate picture possible. Depending on the regulatory agency, the standard for what is deemed an “adequate” size for a provider network will differ, but one important aspect remains the same. It is impossible to calculate the geographic network adequacy of a plan without the help of a GIS. Still, this is not a trivial matter when one considers the math involved. The number of calculations for this, from the individual perspective, is daunting, on the order of 34 billion for a medium-sized health plan.
But what about going back to the patient perspective on the question of access to healthcare? There are now regulations in place that attempt to improve access to care by first understanding it from the patient’s perspective. I’m talking about network adequacy requirements, which refer to a health plan’s (including provider/plans) ability to deliver the benefits promised by providing reasonable access to a sufficient number of in-network primary care and specialty physicians, as well as all healthcare services included under the terms of the contract. Given the vast differences in topologies and road networks from one place to another, it makes sense that the regulation is based on driving times and driving distances together to formulate the most accurate picture possible. Depending on the regulatory agency, the standard for what is deemed an “adequate” size for a provider network will differ, but one important aspect remains the same. It is impossible to calculate the geographic network adequacy of a plan without the help of a GIS. Still, this is not a trivial matter when one considers the math involved. The number of calculations for this, from the individual perspective, is daunting, on the order of 34 billion for a medium-sized health plan.
A broader view of access
While the example exposes the power of modern GIS tools, one should also look beyond the network adequacy calculation and use the resultant data to help optimize networks and provide better care and services to the population. GIS and its analytic capabilities make it easy to assess disparities, identify root causes, and intervene strategically to answer important questions. Where are there gaps in the network? What other services are needed? How can we improve the network? Where can I target my workforce recruitment efforts?
Geographic access has come a long way in the past two decades. Modern technology makes it possible to address all geographic aspects of access—from network adequacy for health plans and service areas for hospitals to program access for public health and universal health coverage for sustainable development. But geographic accessibility is just one component of access. While the Institute of Medicine report mentioned only three components of access, many organizations count five A’s of access: affordability, availability, accessibility, accommodation, and acceptability. And even though geography is called out in only one of these criteria, I can certainly imagine how a GIS might add value to all five.
Health service access is one of the most critical and foundational aspects of our health systems. Advances in access calculations are helping to paint a more realistic picture of access for all. But we’re not there yet. Broader thinking about the social determinants of health and multimodal travel options further complicate how we choose to calculate and regulate access to ensure equity and better health for all. Those forward thinkers are defining a new access term—travel burden—to account for issues like vehicle ownership, transportation types, disability, and financial status. I, for one, am optimistic about the value that GIS brings and will continue to bring as we sort out the challenges of access to health services for everyone, everywhere.
To learn more about improving healthcare access with GIS, watch this video, review this webinar, and visit esri.com/health.
About the Author
Estella M. Geraghty, MD, MS, MPH, CPH, GISP, is the Chief Medical Officer at Esri.